I'm K. Sai likhitha a medical student from India. Here in this blog i share my personal learning experience in medicine department beginning from my first patient practical interaction.
This elog has been created after taking the consent from the patient and their relatives. Links to some of the logged case reports are attached along with my personal patient experience and learning outcome from that particular case.
My experience with the case based blended ecosystem in medicine department has been very unique and transitional with time. Initially when i have seen our professors and interns discussing the cases through an online call during my second year of MBBS, i was very enthusiastic and interested but I have no idea about anything at that time. After a couple of similar online calls, my eagerness and interest has started sloping down and the only thing i have learnt during that time was to get aware of most of the terminology. It was almost more than one Android half year( due to covid) after joining in the first year of MBBS i have seen something like this and it really felt like the actual medicine training is gonna start from now. And from then it took a few more months to practically see the patients personally in the wards and talk to them.
First personal patient encounter
Link to the case: https://www.blogger.com/blog/post/edit/6532713601891436629/4849626673101142178
This is the case of a 34 year old female with recurrent vomitings since 6 months. Initially i was surprised that why does the vomiting didn't bother her at all since 6 months, eventually after seeing more patients i registered that pain is the ultimate thing that brings a person to the clinic. Many patients are concerned only when the symptoms are troubling their daily routine until then they don't want to visit the hospital. This patient even though she had vomitings since 6 months she came to hospital because the frequency of vomiting has increased and she could not perform her work due to weakness.
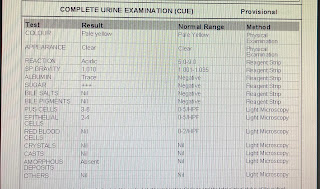
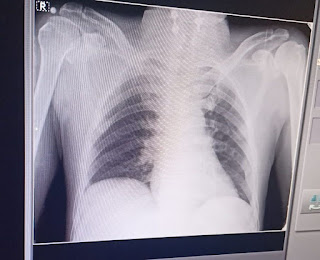
She was very thin built and on examination pallor was present. Her blood pressure was 110/60 mm hg. The provisional diagnosis was acute hypertension secondary to dehydration and vomitings.
This helped me improving my history taking skills and communication with the patients. I have also learned how the dehydration due to vomitings can cause the secondary hypertension with its effects on cardiac and renal systems.