This is an online e log book to discuss our patient de-identified health data shared after taking his / her / guardians informed consent. Here we discuss our individual patients problems through series of inputs from available global online community of experts with an aim to solve those patients clinical problem with collective current best evident based input.
This E blog also reflects my patient centered online learning portfolio and your valuable inputs on the comment box is welcome.
I have been given this case to solve in an attempt to understand the topic of " patient clinical data analysis" to develop my competency in reading and comprehending clinical data including history, clinical findings investigations and come up with diagnosis and treatment plan.
History of presenting illness:
Fever since 7-days high grade-not associated with chills and rigor, evening rise + Associated with sweating
Cough since 7- days associated with less amount of sputum, mucoid. blood tinged aggravated on changing position from lying down to sitting position, no reliving factors
SOB grade - I MMRC -: 7 days more associated with cough, relieved on rest not associated with wheeze
NO H/O similar complaints in the past
No past H/O TB, loss of appetite, loss of weight
K/C/O: Dm+ since 2years
N/K/C/O HTN,CAD ,Br Asthma ,epilepsy
H/o RTA 1 1/2 year back
Fracture of neck of femur with dynamic hip screw surgery done in outside Hospital.Immobilisation 1 month to 1-1/2 year back
- H/o -electrocution
4-years back - Burns both hands
PERSONAL HISTORY
Patient is Binge Alcoholic and Smokes 18 cigarettes in a day later he started smoking Bedi Suttas(high tobacco cigar) in day.
Patient attendant said that their neighbour has TB ( who is son in law of him )
And Patient visits weekly 4 times to his home & spend with him approximately 1-hour a day
Patient started to have fever since 10 days at night time with burning sensation all over the body
Patient started to have unbearable pain at lower back during cough .and always needed help from attendants to hold his back during coughing.
PAST HISTORY
K/c/o DM since 2 years was diagnosed during his RTA treatment and is on regular Glimiperide 1mg &Metformin 500mg medication since then.
He has no history of hypertension, diabetes ,asthma, epilepsy, tuberculosis.
GENERAL EXAMINATION
Patient is conscious, cooperative ,coherent and oriented with time , place , date.
Slightly pallor,
No icterus, cyanosis, clubbing, lymphadenopathy, edema was noted





















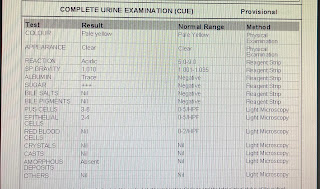









No comments:
Post a Comment